Complications of Dental Implants
Complications Caused by Missing Teeth
Proper oral hygiene and regular dental visits can significantly improve your oral health and keep your pearly whites healthy. Yet, tooth loss may still occur due to various reasons like injury, tooth decay, gum disease or other complications.
Since missing teeth can have many negative impacts on different aspects of your life, they need to be replaced. A missing tooth can cause bone loss and affect your facial structure, the beauty of your smile, confidence, and even speech patterns.
Missing teeth can also cause damage to the adjacent teeth. If missing teeth are not replaced soon enough, the adjacent teeth may shift and cause new dental problems like crooked teeth, crowded teeth, or gapped teeth.
The good news is that your dentist can offer different options as a missing tooth replacement, so you won’t have to live with the inconvenience and embarrassment of a compromised smile.
What Are Dental Implants?
Replacement for Missing Natural Teeth
Dental implants replace your tooth roots and provide a strong base for an artificial tooth. A dental implant is a screw-like post surgically implanted into your jawbone to substitute for the tooth’s root. During dental implant surgery, your dentist will place an abutment (a connector) on top of your dental implant to connect it to the replacement tooth (dental crowns). Your gum tissue will close around the implant. Your dentist will finish the dental implant surgery by placing a dental crown on the abutment.
A dental implant prepares a solid foundation for an artificial tooth.
The artificial teeth will mimic the look and function of your natural teeth.
What Are the Risk Factors and Complications of Dental Implants?
Success Rate of Dental implant Treatment
While dental implants have achieved a high success rate in dentistry, around 90 to 95 per cent, risks and complications can always occur.
Dental implant surgery may fail either at the early stages and shortly after the procedure or months or years later. Implant survival depends on many factors; dental implant complications may be patient-related or implant-related.
Dental implant failure may also occur due to poor planning before the implant procedure and the oral surgeon or dentist’s failure to conduct a comprehensive and well-detailed preoperative assessment. An accurate and complete treatment plan can be highly effective in preventing dental implant failure.
The detailed analysis should entail an in-depth medical history, a planned prosthetic design, and a clinical, radiographic examination.
Implant Dentistry: Early Complications
In some cases, dental implant failure occurs shortly after dental implant placement due to various reasons. Early dental implant failure can happen within the first four months of implant placement.
Below we have provided some possible complications leading to early implant failure.
Presence of Infection at the Implant Site
Bacterial colonization on the surface of the dental implant can result in the early loss of the dental implant. Smoking, autoimmune diseases, and bad oral hygiene can elevate the risk of complications.
Micro Movements of the Dental Implants
Dental implants should be stable and immobile so that the osseointegration can occur properly. If the replacement teeth are placed immediately after dental implant procedures, micro-movements of the dental implants can be expected.
The oral surgeon will not typically place the artificial tooth replacement right after the dental implant surgery. Your jaw bone should have enough time to integrate with the dental implant properly.
While placing immediate tooth replacements will reduce the number of visits to the clinic, it can increase the risk of complications and eventually lead to dental implant failure.
However, carefully selected cases for immediate tooth replacement can have successful outcomes.
Failed Osseointegration
Failed or impaired osseointegrated dental implants can lead to the early loss of the dental implant. The impaired osseointegration process might occur due to the lack of intimate connection between the bone and the dental implant.
Failed osseointegrated implants mean dental implants have not fully integrated with the jawbone. Poor osseointegration can cause dental implants to loosen or dislodge.
The absence of adequate bone to support a dental implant can be a risk factor for failed osseointegration process. The dentist or oral surgeon should ensure that you have sufficient bone density and have healthy gums and bones before beginning the dental implant procedure.
Insufficient bone to support dental implants can lead to dental implant failure; dental professionals should perform bone grafting in this situation.
A bone graft procedure is done to stimulate more bone growth.
Allergic Reactions
If you are allergic to titanium, you may experience an allergic reaction to your dental implant since most dental implants are made up of a biocompatible metal called titanium.
Loss of taste, having a tingling sensation, and swelling may be signs of allergic reactions.
Your dentist may offer dental implants from different materials if you inform them about your allergy.
Not Following the Dentist’s Post-Operative Instructions
There are many factors involved that can lower the risk of complications and increase the survival chance of dental implants.
Your dentist may ask you to avoid certain activities and stick to soft foods for the first few days or weeks after dental implant surgery to accelerate the healing process.
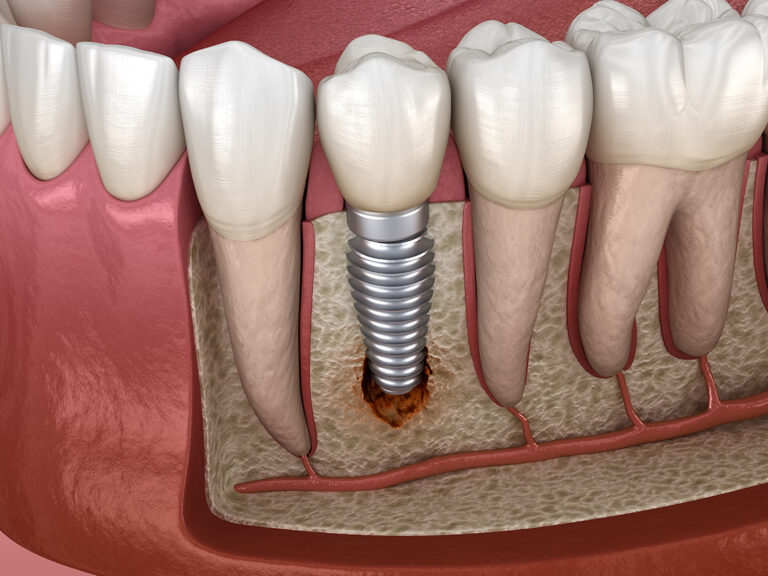
Implant Dentistry: Late or Long-Term Complications
Sometimes dental implant surgery may be a success initially and turn into a failure in the long run.
Late dental implant failure can be defined as the reduction of stability of dental implants after about six months.
Many factors are involved, such as:
- bone quality and quantity
- plaque accumulation around the implant
- bad oral hygiene
- periodontal disorders
Let’s see some of the problems and complications that can arise months or years after implant surgery.
Nerve or Tissue Damage
Nerve damage is a probable complication of dental implant surgery if the implant has been placed too close to the nerves.
Nerve damage can occur due to poor and inaccurate treatment planning before dental implant procedures. Experienced dentists will locate the nerves by taking x-rays before the procedure, determining the best position for the
implant placement to avoid possible complications after implant surgery.
Tingling sensations in the gums, face, lips, or tongue and persistent pain or discomfort could indicate nerve damage. Nerve injury, especially to the inferior alveolar nerve, can be a serious issue that requires immediate care.
Foreign Body Rejection
While not very common, your body may reject the metal implant post. Some people have a slight sensitivity to metal, leading to this complication. Foreign body rejection can have signs like fever, pain at the implant site, and swelling.
Sinus Damage
Implant placement in the upper jaw may sometimes challenge oral and maxillofacial surgeons. Dental implants placed in the upper jaw may protrude into the sinus cavities leading to discomfort or infection.
Infection caused by an implant protruding in the sinus can have symptoms such as :
- swelling of the sinuses
- fever
- Pain similar to toothache
- headache
- stuffy nose
- compromised sense of smell
Loosening of Dental Implant
Dental implant surgery can turn into a failure due to the loosening of dental implants. Trauma and injury around the implant can cause the implant to become loose.
Peri-Implant Diseases
Peri-implant diseases refer to inflammatory conditions that can damage tissues and bone leading to the failure of dental implants. The most common cause of the condition is typically poor oral hygiene, smoking, gum disease, or periodontitis history.
Bacterial accumulation on the surface of dental implants causes inflammation of the mucous membrane around the implant. This stage is referred to as peri-implant mucositis.
A more severe and dangerous condition known as peri-implantitis can result from untreated peri-implant mucositis. Peri-implantitis is associated with greater inflammation than peri-implant mucositis, and the patient will experience bone loss around dental implants.
Having a history of periodontitis(advanced stage of gum disease) can significantly elevate the risk of peri-implantitis and, consequently, dental implant failure.
The dental professional should examine your mouth, gums, and other teeth to ensure the procedure suits your situation.
It’s imperative to maintain your gums and natural teeth healthy to avoid complications with dental implants.
Patient-Related Complications of Implant Surgery
As mentioned earlier, dental implant surgery, like any other dental surgery, includes risks and complications and may fail due to several factors.
Some of these risk factors are common complications of all dental procedures, some are associated with the dentist or oral surgeon’s poor planning, and some are caused by the patient.
Here are some common factors related to the patient that can lead to dental implant failure:
Patient-Related
- Smoking
- Teeth grinding
- Improper dental hygiene
- Medical conditions
- Insufficient jaw bone
- Allergic reactions
*Patients who smoke may experience insufficient bone healing in the surgical site due to compromised blood circulation.
*Teeth grinding or bruxism can cause dental implants to break, crack, or loosen due to excessive force and pressure.
*Some medical conditions like diabetes may also increase the risk of complications after implantation of dental implants.
*Dentists may perform bone grafting to increase bone density. The bone graft could be from the patient’s body or a synthetic. Bone grafting encourages new bone growth and increases the chance of dental implant success.
Implant-Related
Some studies have also related some dental implant surgery complications to the implant and not the patient.
Based on some research, shorter implants will typically face more failure than longer implants. Longer implants seem to have an increased chance of success, probably due to having a larger contact surface with the bone.

After Dental Implant Surgery
You may experience these symptoms following your implant placement:
- minor bleeding
- swelling in the gum tissue or your face
- pain or discomfort at the surgical site
- infection of dental implants
- an opening of the incision after surgery
Your dentist or oral surgeon may prescribe pain medications to alleviate the pain and swelling. You are also recommended to eat soft foods for a few days following surgery so that the surgical site can heal properly.
Damage to blood vessels and the surrounding teeth is another complication of dental implant placement.
How do you know if a dental implant is failing?
Signs Of Dental Implant Failure
The following symptoms can indicate that dental implant surgery has been a failure.
- the dental implant is mobile and loosened
- bone loss
- receding gums
- pain or discomfort, especially upon tapping the dental implant
- trouble chewing
- pus coming from the surgical site
Who Performs Dental Implants?
Dental implants in Brisbane are a team-effort procedure.
Oral and maxillofacial surgeons perform implant placement.
Periodontists are also involved in the procedure to deal with the prevention and treatment of gum disease.




































